This guide explains what home oxygen is, who it is for, how it is set up, and how to use it safely.
What is oxygen therapy at home?
Oxygen therapy at home is the use of medical oxygen to raise a person’s blood oxygen to a safer range. It is delivered through equipment such as an oxygen concentrator or oxygen cylinders, usually via nasal cannulae or a face mask.
It is different from a fan, inhalers, or general “air” support. Oxygen is a medicine, so it should be used exactly as prescribed.
Who is home oxygen therapy for?
Home oxygen is typically prescribed for people with confirmed low oxygen levels (hypoxaemia). This is commonly linked to conditions such as COPD, pulmonary fibrosis, severe asthma, bronchiectasis, heart failure, pulmonary hypertension, or certain neuromuscular disorders.
Not everyone who feels breathless needs oxygen. Breathlessness can happen even when oxygen levels are normal, which is why assessment matters.
How do clinicians decide if someone needs oxygen?
Clinicians usually decide using objective testing, not symptoms alone. They may measure oxygen saturation with a pulse oximeter and confirm with an arterial blood gas test, especially when long-term oxygen is being considered.
They may also assess oxygen levels during sleep and exertion because some people desaturate mainly at night or when walking. The prescription will specify the flow rate and when oxygen should be used.
What types of home oxygen equipment might they be offered?
Most people are offered one of three main options, sometimes in combination. The right setup depends on prescription, lifestyle, and how much oxygen they need.
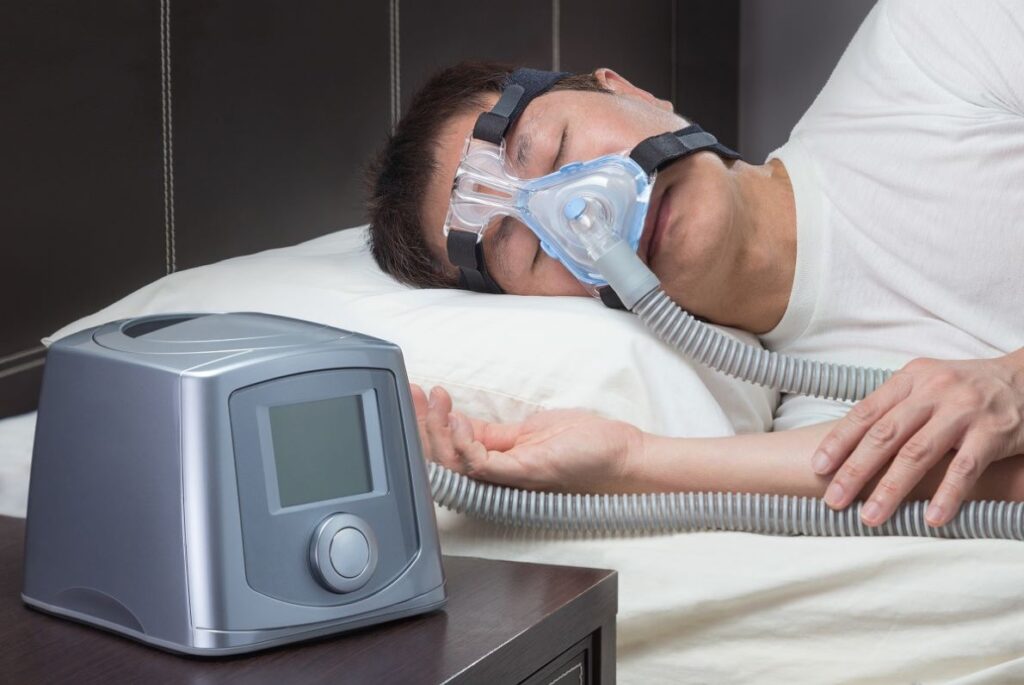
A stationary oxygen concentrator is the most common for home use. It pulls oxygen from room air and provides a continuous supply without deliveries, but it needs electricity and regular maintenance.
Oxygen cylinders provide portable or backup oxygen. They are useful for power cuts or short outings, but they require deliveries and safe storage.
Portable oxygen concentrators may be offered for travel and mobility. Some provide pulse dose oxygen rather than continuous flow, so they are not suitable for everyone.
How is oxygen delivered to the person?
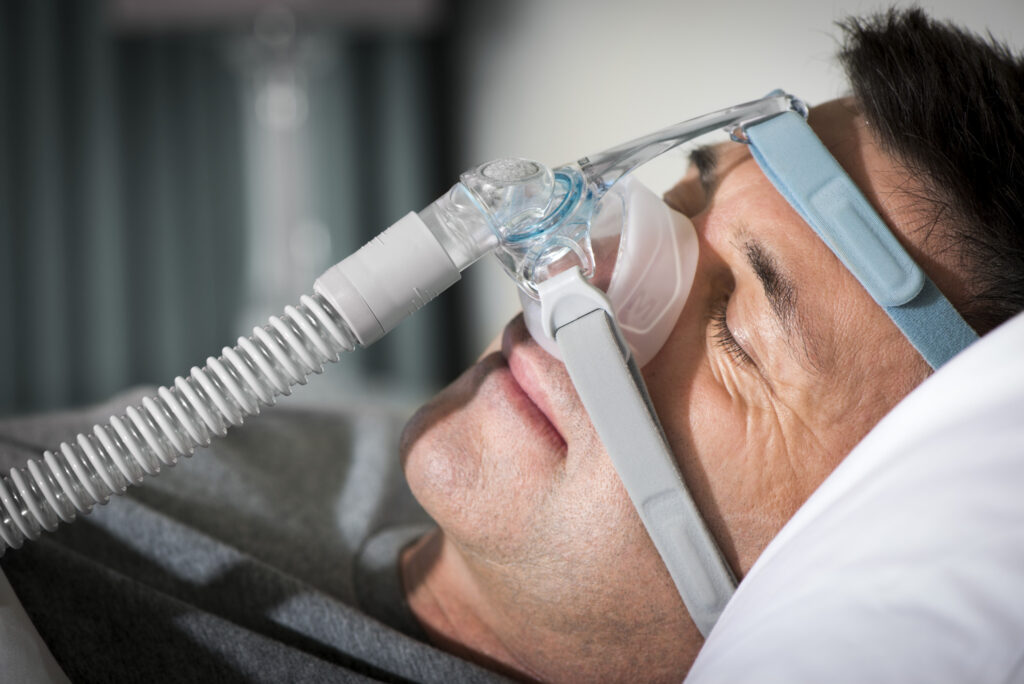
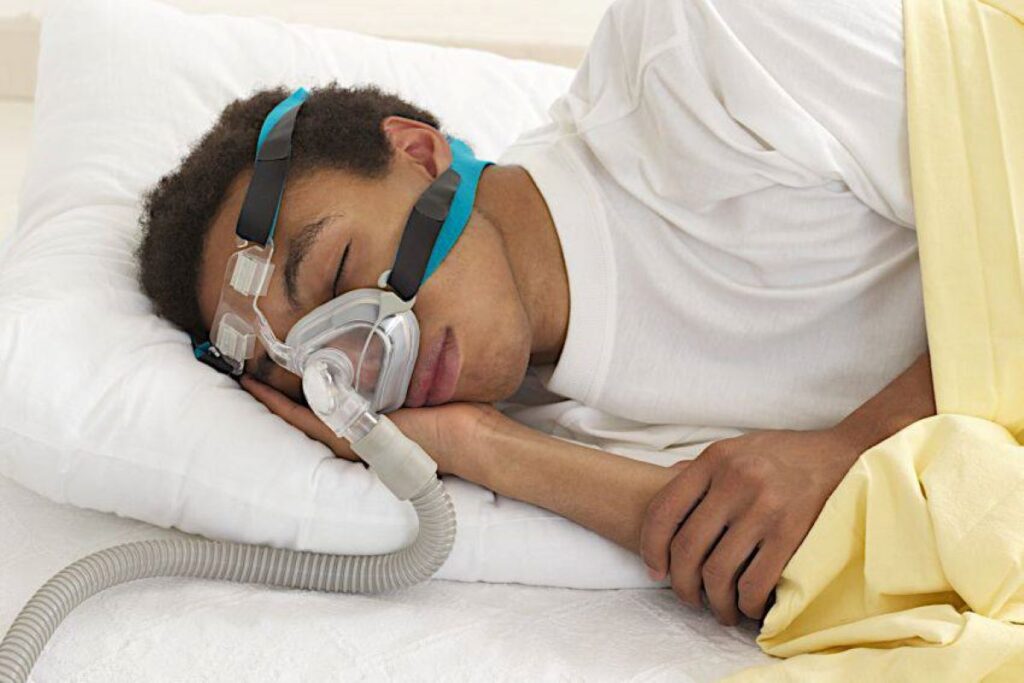
Oxygen is most commonly delivered through nasal cannulae, which sit just inside the nostrils. They are usually more comfortable for longer wear and allow eating and talking.
A face mask may be used when higher flow rates are needed or if nasal cannulae are not tolerated. Some people may have humidification added if their nose or throat becomes dry, depending on flow rate and comfort.
How do they use oxygen correctly day to day?
They should follow the prescription exactly, including the flow rate and the times they should use it. Changing the flow “to feel better” can be unsafe, especially for some people with chronic lung disease.
They should check that tubing is connected securely, that the device is running properly, and that cannulae or masks are positioned comfortably. If they have a target saturation range from their clinician, they should aim for that rather than chasing a high number.
They should also plan movement around the home to avoid pulling on tubing, and keep the tubing length appropriate to reduce trip hazards.
What safety rules matter most at home?
The most important rule is no smoking and no naked flames near oxygen. Oxygen itself is not flammable, but it makes fires start more easily and burn far more fiercely, including with cigarettes, candles, gas hobs, and e-cigarettes.
They should keep oxygen equipment away from heat sources and ensure good ventilation around concentrators. Greasy creams and petroleum-based products should be avoided on the face or in the nose, as they can increase fire risk; water-based alternatives are usually preferred.
They should secure cylinders upright, store them safely, and keep equipment clear of clutter. If they use oxygen while cooking, they should follow their oxygen provider’s guidance and consider practical adjustments to reduce risk.
What are common side effects and how can they be managed?
Dryness of the nose and throat is common, especially with higher flows. They can often manage this with good hydration, correct cannula fit, and clinician-approved moisturisers that are not oil-based.
Skin irritation can occur where tubing touches the cheeks or ears. Soft covers, repositioning, and regular cleaning of equipment may help.
Some people feel anxious when starting oxygen. Clear instructions, a simple routine, and reassurance that breathlessness can have multiple causes can make the transition easier.
How should they monitor progress and know when to ask for help?
They should contact their clinician if symptoms worsen, oxygen requirements change, or they experience new confusion, severe drowsiness, chest pain, blue lips, or a sudden drop in saturation if they have been advised to monitor it. They should also seek help if equipment alarms persist or if oxygen delivery seems unreliable.
Routine follow-ups matter because oxygen needs can change over time. Clinicians may reassess oxygen levels, update flow rates, and confirm whether oxygen is still needed at the current schedule. For cost insights, see this guide on portable oxygen concentrator prices in Australia and what affects them.
What should they know about travelling and going out?
They should plan ahead, especially if they need oxygen outside the home. That may include arranging portable oxygen, checking battery life for portable concentrators, and ensuring they know how long a cylinder will last at their flow rate.
For car travel, equipment should be secured and kept away from heat. For flights, they usually need airline approval and an appropriate portable concentrator; oxygen cylinders are generally not permitted on commercial flights. Oxygen providers can often advise on travel arrangements.
What is the simplest way to get started?
They should start with the prescription, a clear demonstration of equipment use, and a written safety checklist. A good first week focus is simple: use oxygen at the prescribed times, keep it away from flames and smoking, reduce trip hazards, and note any issues to discuss at follow-up.
Used properly, home oxygen can support daily life, but it works best when it is treated like any other medicine: correctly, consistently, and safely.
FAQs (Frequently Asked Questions)
What is home oxygen therapy and how does it work?
Home oxygen therapy involves using medical oxygen to raise a person’s blood oxygen levels to a safer range. It is delivered through equipment such as oxygen concentrators or cylinders, typically via nasal cannulae or face masks. This therapy helps reduce breathlessness, improve sleep, and support daily activities when used correctly as prescribed.
Who is eligible for home oxygen therapy?
Home oxygen therapy is prescribed for individuals with confirmed low blood oxygen levels (hypoxaemia), often linked to long-term conditions like COPD, pulmonary fibrosis, severe asthma, bronchiectasis, heart failure, pulmonary hypertension, or certain neuromuscular disorders. Not everyone who experiences breathlessness requires oxygen; proper assessment is essential.
How do clinicians determine if someone needs home oxygen?
Clinicians use objective tests such as pulse oximetry and arterial blood gas analysis to measure oxygen saturation levels. They may also assess oxygen levels during sleep and physical exertion to identify desaturation episodes. Prescriptions specify the appropriate flow rate and timing for oxygen use based on these assessments.
What types of equipment are used for home oxygen therapy?
Common equipment includes stationary oxygen concentrators that provide continuous oxygen supply at home, portable oxygen concentrators for mobility and travel (which may deliver pulse dose oxygen), and oxygen cylinders used as portable backup or during power outages. The choice depends on prescription needs, lifestyle, and required oxygen flow.
What safety precautions should be followed when using home oxygen?
Key safety rules include avoiding smoking or naked flames near oxygen equipment since enriched oxygen increases fire risk. Equipment should be kept away from heat sources with good ventilation around concentrators. Greasy or petroleum-based products on the face or nose should be avoided. Cylinders must be stored upright securely, and trip hazards from tubing should be minimised.
How can users manage common side effects of home oxygen therapy?
Dryness of the nose and throat can often be relieved by staying well hydrated, ensuring correct cannula fit, and using clinician-approved moisturisers that are not oil-based. Skin irritation from tubing contact can be managed with soft covers, repositioning equipment regularly, and maintaining cleanliness. Anxiety about starting oxygen may improve with clear instructions and reassurance.